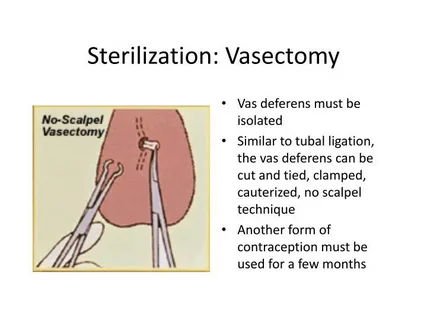
The no scalpel vasectomy has become one of the most trusted, minimally invasive options for permanent male contraception. Compared to traditional vasectomy techniques, the no scalpel method reduces incision size, lowers complication rates, shortens recovery time, and improves overall patient comfort. Yet despite the efficiency of the procedure itself, the confirmation of sterility remains a critical step that many patients struggle to complete.
Following a no scalpel vasectomy, men must undergo semen analysis to ensure that sperm are no longer present in the ejaculate. Historically, patients have had to visit a clinic or laboratory for post-vasectomy semen testing—a process that many find inconvenient or embarrassing. As a result, a significant number of men skip or delay testing, placing themselves and their partners at risk of unintended pregnancy.
This gap in follow-up care has driven the rise of automated semen analysis kits, a transformative innovation that allows men to verify sterility from the comfort of home. These kits integrate digital technology, optical sensors, smartphone connectivity, and automated analysis algorithms to provide fast, privacy-friendly, and highly accurate results.
This article explores how automated semen analysis kits are reshaping the no scalpel vasectomy experience, improving compliance, and supporting better reproductive outcomes.
1. Why Semen Analysis Is Essential After a No Scalpel Vasectomy
Although a no scalpel vasectomy is highly effective, sterility is not immediate. Sperm can remain in the vas deferens and seminal vesicles for weeks or even months after the procedure. To ensure contraception works as intended, patients must submit at least one, and sometimes two, semen samples showing azoospermia (no sperm) or rare non-motile sperm.
Skipping this step is dangerous, yet common. Reasons men skip testing include:
- Inconvenience of traveling to a clinic
- Embarrassment about dropping off a sample
- Time constraints due to work or family
- Lack of understanding about the importance
- Forgetfulness during the recovery period
Automated semen analysis kits eliminate these barriers by allowing post-vasectomy testing at home.
2. What Are Automated Semen Analysis Kits?
Automated semen analysis kits are at-home diagnostic tools designed to evaluate semen samples digitally, without requiring manual microscopic review. They use advanced technologies such as:
• Optical imaging sensors
These sensors capture high-resolution images of the semen sample.
• Motion-tracking algorithms
Integrated software detects and measures sperm motility.
• Machine learning–based classification
AI models assess sperm concentration and categorize results.
• Smartphone connectivity
Most kits pair with a phone app to guide the process, display results, and store data.
• Encrypted data systems
Results remain private and can be shared with a clinician only if the patient chooses.
These kits provide a reliable, user-friendly way to verify sterility following a no scalpel vasectomy.
3. How Automated Semen Analysis Kits Work
While different brands vary in design, most automated semen analysis systems follow this workflow:
Step 1: Sample Collection
The patient collects a semen sample in a sterile cup provided in the kit. Instructions guide abstinence periods and technique to ensure accuracy.
Step 2: Slide or Cartridge Preparation
A small amount of semen is placed on a test slide or into a microfluidic cartridge that controls flow and distributes the sample evenly.
Step 3: Device Insertion
The slide or cartridge is inserted into:
- A handheld optical scanner
- A smartphone-attached lens module
- A compact digital analyzer
Depending on the system, the smartphone camera or internal sensors capture data.
Step 4: Automated Image and Motion Analysis
The device’s software evaluates:
- Sperm count
- Sperm motility
- Presence of rare non-motile sperm
- Sample quality
This analysis is typically completed within 5–10 minutes.
Step 5: Digital Results
The results are displayed instantly in the smartphone app, showing whether sperm are detected. A visual or numeric scale may indicate:
- Azoospermia: No sperm detected
- Low sperm count: Rare non-motile sperm
- Motile sperm present: Not yet cleared
Men can repeat the test at recommended intervals or share data with their healthcare provider.
4. Advantages of Automated Semen Analysis Kits in No Scalpel Vasectomy Care
1. Increased Follow-Up Compliance
One of the biggest benefits is dramatically improved adherence. When patients can test from home:
- No travel is needed
- No embarrassment is involved
- Testing feels more private
- Scheduling is flexible
This leads to higher sterility confirmation rates.
2. Faster Clearance
Since testing is easier, men typically perform semen analysis sooner, helping them transition to unprotected intercourse earlier with confidence.
3. High Accuracy
Modern automated systems have accuracy levels comparable to laboratory microscopy for detecting sperm presence or motion.
4. Reduced Clinic Burden
Urology practices benefit from:
- Fewer clinic visits
- Reduced sample processing
- Streamlined workflow
- More time for surgical appointments
5. Better Patient Experience
Patients appreciate the convenience and modern feel of technology-driven testing.
6. Easy Digital Record Keeping
The app stores results automatically, creating a complete timeline and allowing clinicians to review data if needed.
5. The Technology Behind Automated Semen Analysis
Technological advancement has made at-home semen testing more sophisticated than ever before.
a. Microfluidic Chip Design
Microchannels allow semen to flow in a controlled environment, improving imaging and preventing clumping.
b. Smartphone-Enhanced Microscopy
High-resolution phone cameras, combined with precision lenses, can match laboratory-grade imaging.
c. AI and Computer Vision
Machine learning algorithms identify sperm in real time and evaluate:
- Count
- Motility
- Behavioral patterns
d. Cloud Connectivity
Secure cloud systems store results for long-term monitoring.
e. Automated Quality Control
The system can detect:
- Sample inconsistencies
- Insufficient volume
- Presence of debris
This reduces user error.
These technological innovations allow accurate, high-speed analysis outside of clinical settings.
6. The Role of Automated Kits in Modern No Scalpel Vasectomy Protocols
More urology clinics are integrating automated semen testing into their standard care pathways. This modernizes the no scalpel vasectomy experience in several ways:
1. Remote Postoperative Care
Patients no longer need multiple follow-up visits. Semen testing, education, and messaging are handled digitally.
2. Increased Safety
Automated alerts can notify men when motile sperm remain and advise continued contraception.
3. Streamlined Sterility Clearance
Systems automatically confirm when semen is sperm-free, reducing administrative work for the clinic.
4. Reduced Anxiety
Men feel more informed and reassured with immediate, easy-to-interpret results.
5. Enhanced Patient Engagement
Apps often provide educational content, reminders, and step-by-step instructions.
As a result, automated semen analysis kits are becoming a powerful complement to the minimally invasive no scalpel vasectomy technique.
7. Challenges and Limitations of Automated Semen Analysis Kits
While promising, these systems are not without limitations.
a. Cost
Some kits can be more expensive than traditional lab testing, though prices are decreasing with wider adoption.
b. Technology Literacy
Not all patients feel comfortable with smartphone-connected devices.
c. Variability in Accuracy
Although highly accurate for sperm detection, some kits may not measure subtle nuances of motility as precisely as a laboratory.
d. Single-Use Designs
Many kits are disposable, requiring repurchase for multiple tests.
e. Limited Regulatory Oversight in Some Regions
Not all kits undergo standardized validation, making brand selection important.
Despite these challenges, most patients find automated testing significantly easier and more convenient.
8. Future Innovations: What’s Next for Post-Vasectomy Testing?
The next generation of automated semen analysis technology is expected to include:
• AI-enhanced predictive fertility clearance
Systems will estimate when a patient will achieve azoospermia based on early sample data.
• Integration with wearable devices
Tracking recovery data such as temperature or inflammation may optimize follow-up timing.
• 5G-enabled real-time clinician review
Doctors could instantly verify images or provide recommendations.
• Fully disposable micro-diagnostic pods
These will eliminate the need for device cleaning or reassembly.
• Multiplatform reproductive health dashboards
Apps will integrate vasectomy data with long-term male health monitoring.
• Advanced motility detection algorithms
These may surpass human technicians in detecting subtle sperm movement patterns.
As technology improves, at-home semen analysis may become the worldwide standard of care after a no scalpel vasectomy.
Conclusion
The no scalpel vasectomy has revolutionized male contraception by offering a minimally invasive, low-risk, and highly effective procedure. Yet postoperative semen analysis remains essential for confirming sterility. Automated semen analysis kits bridge the gap between procedure and confirmation, allowing men to complete this step conveniently, privately, and accurately at home.
These digital tools enhance follow-up compliance, improve patient satisfaction, reduce clinic burden, and ensure safer contraceptive outcomes. As technology advances, automated semen analysis kits will play an even more central role in the future of no scalpel vasectomy care—bringing together precision, convenience, and modern healthcare innovation.
FAQs
1. Are automated semen analysis kits as accurate as laboratory testing?
Most high-quality kits provide accuracy comparable to lab microscopy for detecting sperm presence and motility. They are reliable for post-vasectomy clearance but may not replace clinical fertility evaluations.
2. How soon after a no scalpel vasectomy can I use an automated test?
Most urologists recommend testing 8–12 weeks after the procedure or after 20–30 ejaculations. Always follow your surgeon’s specific timeline.
3. Do I need multiple tests to confirm sterility?
In many cases, one azoospermia result is enough. However, some clinics require two negative tests. Automated kits make it easy to perform multiple tests from home if needed.